“I Ate Pages from My Passport After Being Denied Food at Mohlomi Hospital”
26 February 2024 by Lerato Matheka
Est Read Time: 12 min(s) 19 sec(s)
Listen to this article:
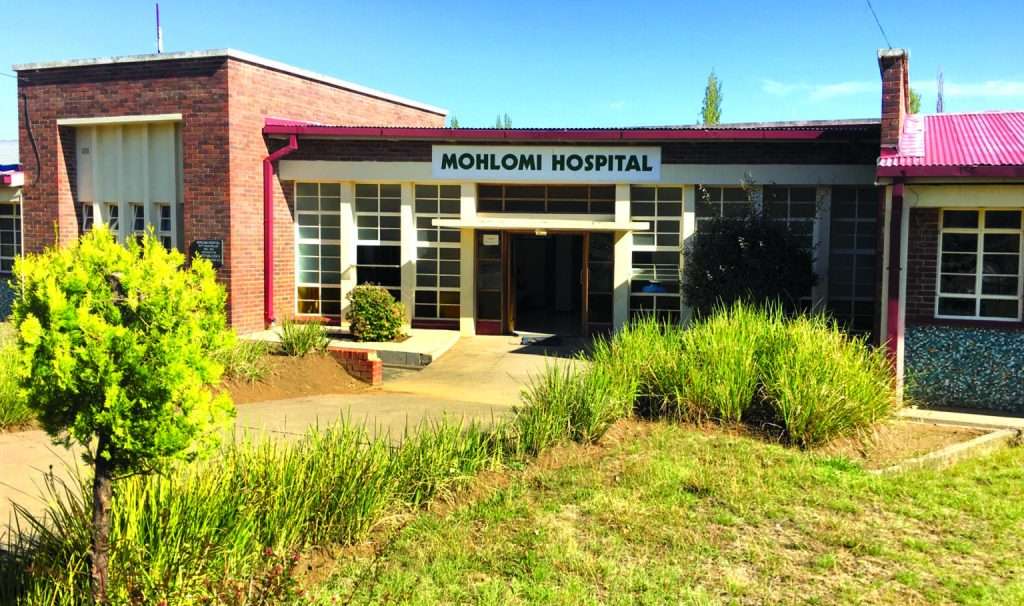
Mohlomi Mental Hospital stands accused of abusing patients. Management promises to investigate abuse allegations. Credit: Newsday
With each crinkle, *Reitumetse Mohai’s throat emitted a subdued, rasping noise as she swallowed pages of her passport.
At the age of 37, Reitumetse found herself admitted to Lesotho’s only mental hospital, Mohlomi in Maseru, at the beginning of 2022.
Upon her arrival, she was promptly taken and confined in a seclusion room—a specially designated area within a psychiatric facility or hospital where patients can be isolated.
At Mohlomi Hospital, the seclusion room measures approximately 2×2 square metres, equipped with a cement bed and lacking a mattress or toilet facility for isolated patients.
The seclusion room, equipped with a heavy steel door that closes from the outside and partially broken rectangular window covered in barbed wire, exposes patients to various weather conditions, including the freezing winter cold. Although nurses deliver food through a small opening in the door, patients claim it is not a daily occurrence.
Mohlomi Mental Hospital’s senior nursing officer, Maholi Rampeta, stated that the seclusion room is designated for patients who are highly disturbed and pose a risk to themselves, other patients, and staff.
In October 2023, Advocate Tlotliso Polaki, the Ombudsman, issued a scathing report on Mohlomi Mental Hospital, highlighting it as a neglected facility.
The report emphasised that conditions at the hospital, exacerbated by a shortage of resources, were deteriorating, and adversely affecting the well-being of patients.
“The living conditions at Mohlomi are inhumane and violate the fundamental human rights of the patients, as outlined in various domestic and international standards and agreements. The Ombudsman has found that these dire conditions hinder the improvement of their mental health due to the poor quality of care they receive,” Advocate Polaki said.
These violations of fundamental human rights are detailed by Reitumetse, who was confined in a seclusion room, isolated, and deprived of food for five days.
As each passing hour, Reitumetse’s stomach rumbled louder. With a desperate search around her, the only edible thing she could find was the pages of her passport.
With each tear, every page surrendered to her grasp, the sound of ripping paper echoing in the silence of her hunger-stricken room.
As she swallowed each morsel, the dry parchment scratched against her throat, a bitter reminder of the lengths she would go to stave off starvation.
“My hunger was so unbearable that I resorted to eating the pages of my own passport,” Reitumetse said.
She added, “It became my only edible possession for the first two of the five days that I was locked in the seclusion room.” Reitumetse has schizoaffective disorder.
Understanding schizoaffective disorder
A reputable global clinic and research institution, Mayo Clinic, explains schizoaffective disorder as a mental health condition characterized by symptoms from two distinct categories: schizophrenia and mood disorders.
Schizophrenia symptoms can be like seeing or hearing things that are not real, while mood disorder symptoms can include feeling really sad or super excited. It is like having a mix of these two types of challenges at the same time.
“Although the development and course of schizoaffective disorder may vary, defining features include a major mood episode (depressed or manic mood) and at least a two-week period of psychotic symptoms when a major mood episode is not present,” read Mayo Clinic website.
It further explains that there are two types of schizoaffective disorder — bipolar and depression. The bipolar type includes episodes of mania and sometimes major depression, while the depression type, according to Mayo Clinic, includes only major depressive episodes.
Additionally, Mayo Clinic states that signs and symptoms of schizoaffective disorder depend on the type and may include delusions—having false, fixed beliefs, despite evidence to the contrary.
Other symptoms include hallucinations—such as hearing voices or seeing things that are not there; impaired communication and speech, such as being incoherent; bizarre or unusual behaviour; symptoms of depression—such as feeling empty, sad, or worthless or periods of manic mood, with an increase in energy and a decreased need for sleep over several days, and behaviours that are out of character.
Also included in the symptoms are impaired occupational, academic, and social functioning and problems with managing personal care, including cleanliness and physical appearance.
Reitumetse received a diagnosis of schizoaffective disorder when she was a fourth-year student at 21 years old.
“During my episodes, I am either extremely excited, energetic, or irritable,” she said, adding that this makes it difficult to fully realise when she is having an episode.
This is because, at that moment, Reitumetse feels excited and at the peak of her functionality.
“I can go for a day without sleep, but if people try to control me or make me feel violated, I will respond,” explained Reitumetse.
Claims of abuse at Mohlomi Mental Hospital
A large white window adorns the right wing, while the left-wing features marble-like stones beneath another sizable window.
At the centre of these structures stands the entrance, marked by a sign boldly displaying the name “Mohlomi Hospital” in black font.
This aged, red-brick building serves as Lesotho’s sole mental health institution, established by law in 1965 as a national referral facility.
Situated adjacent to Makoanyane Military Base, the hospital welcomes and treats both self-transferred patients and those referred by clinicians from across the ten districts of Lesotho.
However, Mohlomi Mental Hospital is currently embroiled in allegations of numerous human rights violations, including physical, verbal, and emotional abuse.
When reached for comment, the hospital’s senior nursing officer, Maholi Rampeta, was unable to either confirm or deny the allegations of human rights violations.
“I can’t say whether what the patients have told you is true or not. I am very shocked at what is said to be happening,” Rampeta told Newsday. However, she committed to ensuring that all allegations would be thoroughly investigated.
In October 2023, Advocate Tlotliso Polaki, the Ombudsman, issued a scathing report on Mohlomi Mental Hospital, highlighting it as a neglected facility.

Advocate Tlotliso Polaki, the Ombudsman. Credit: Letsoe la Basotho.
The report emphasised that conditions at the hospital, exacerbated by a shortage of resources, were deteriorating, and adversely affecting the well-being of patients.
The Ombudsman’s report was issued more than a year after *Reitumetse Mohai, a patient diagnosed with schizoaffective disorder, was admitted to this hospital.
She alleged that during the first two days of her admission, she was denied food and a blanket while locked up in a seclusion room.
“It was only on the third day that they reluctantly provided me with some food,” revealed Reitumetse, accusing nurses of also denying her access to a bathroom.
“Forced to improvise, I used a plate for relief and the remaining slice of bread to clean myself,” Reitumetse said.
Another patient, *Liteboho Sekhamane, battles with depression and psychosis. This mother of two children is HIV positive and, just like Reitumetse, she claimed that she was denied both food and her antiretroviral medication for days. She claimed nurses are fully aware of her HIV status.
“In 2023, I checked into Mohlomi because I felt my condition was deteriorating. The next day, I woke up in the seclusion room. I don’t remember what happened, but other patients told me I was fine one minute and suddenly started undressing. They say I was walking around naked when I was thrown in there,” Liteboho said.
She strongly feels there was no need to lock her in the seclusion room because “I was not violent towards myself and others.”
She accused nurses at the Mohlomi Mental Hospital of using the seclusion room as a ‘naughty corner’ for patients who need medical attention or those they want to punish.
Liteboho recalled a nurse throwing her medication on the uncleaned seclusion room floor and being instructed to pick and drink the medication.
“This is the floor that every secluded patient urinates and defecates on,” she said.
When the nurse in question returned towards the end of her shift, she once again threw Liteboho’s medication on the floor, threatening her that “they would lock me in there longer if I didn’t take my medication, the same medication she threw on the dirty floor.”
Nurses’ physical abuse
In Liteboho’s memory, one particular case remains deeply ingrained.
“One time, they left me in there for days without food and a blanket. When they eventually came to check up on me, I was motionless. I was so cold, shivering, and couldn’t stomach food or even liquids,” Liteboho recalled.
Instead of receiving assistance, Liteboho claimed that she endured the most severe beating of her life.
“They started beating me, saying I am intentionally acting and refusing to eat. They beat me so much that I had wounds.”
This has driven Liteboho to a point where she declares: “I hate that place.” She expressed disdain for witnessing her medical condition deteriorate to the extent of being admitted to Mohlomi Mental Hospital.
She believes that her assertiveness has labelled her as the number one public enemy at the hospital, as she refuses to take on extra cleaning chores assigned to recovering patients.
“They ask recovering patients to clean up after ailing patients. I always, and will always, refuse to wash another patient’s faeces or even change diapers.
“That stance has subjected me to being given my medication on an empty stomach and being forced to go for days without food. Hear me, all recovering patients are asked to clean up after others.”
When *Reitumetse Mohai was admitted to Mohlomi Mental Hospital in April 2022, she alleged that she was harshly beaten by a nurse. “The slaps were severe and left marks,” she claimed.
She added: “I looked at the nurse, and she had so much anger in her eyes. Her power as she pushed and shoved me outside made it feel as though I was being punished for something huge. Yet, I am told that I climbed on top of a table and started saying I am Jesus and preaching.”
Reitumetse claimed the nurse “certainly slapped me back to reality because the last thing I remembered was sitting and having a conversation with other patients, and suddenly I found myself ducking slaps and punches.”
Despite being aware of the abuse she was enduring, Reitumetse claimed she was dragged to the seclusion room and left there for a few days.
“Spending time in that room has left me with traumatic scars. I can’t sleep in a dark room, and shadows remind me of the scary moments when I was trapped in there,” she said.
Comparing her experiences at Mohlomi Mental Hospital with those of a private facility she previously spent time at, Reitumetse noted that the private facility only sedated her and released her when she woke up.
“With Mohlomi, it seems that seclusion is their admission protocol regardless of one’s condition, and it is definitely their punishment tool,” she alleged.
She claimed that at Mohlomi, individuals with mental illness are unfairly judged and mistreated, while those experiencing depression and suicidal thoughts are placed in a private special ward near the offices.
She stated that her alleged harrowing experiences at Mohlomi Mental Hospital have worsened her already fragile mental health.
Meanwhile, Mohlomi Mental Hospital’s senior nursing officer, Maholi Rampeta, informed Newsday that it was only in rare cases for a patient to stay for more than a week in a seclusion room.
“They need regular medication to help calm them down. They are given injections, and if they complain of pain, they are encouraged to take tablets, which they usually do,” explained Rampeta.
Alleged accounts of misdiagnosis, lack of healing
The ‘Knowledge of Antipsychotic Medication and Their Side Effects among Psychiatric Nurses at a Tertiary Hospital in Lesotho’ is study aimed at describing nurses’ knowledge regarding antipsychotic medications and their side effects at Mohlomi Mental Hospital in Lesotho.
The study indicated that factors impeding the physical health monitoring of patients with severe mental illness are multidimensional. It also stated that healthcare providers’ knowledge and expertise regarding antipsychotic medication and side effects remain key determinants of the frequency and quality of screening a patient shall be subjected to.
“This challenge transcends the monitoring of patients treated with antipsychotics, where scholars have determined a lack of knowledge about screening for adverse effects, resulting in poor clinical assessments among patients prescribed antipsychotics,” read the study published in October 2023.
While the study’s findings conclude that staff at this hospital exhibited fairly good knowledge regarding antipsychotic drugs and their associated side effects, Mohlomi Mental Hospital’s outpatient, *Lieketso Sebolai, claimed she was misdiagnosed twice.
Lieketso’s initial diagnosis was made in South Africa. At the time, she was a student in that country and returned to Lesotho with the confidence that Mohlomi, Lesotho’s only mental health hospital, would be a haven for her.
“That hospital should just shut down because it causes more harm than good,” Lieketso opened her mouth.
“I am one of those patients who are aware of their conditions and know their treatment regimen, so when I was misdiagnosed, I tried to reason. But the last time I was there, I was chased out of the consultation because ‘I knew too much’,” recalled Lieketso.
She claimed that on the two occasions she agreed to take medication prescribed at Mohlomi, she experienced severe relapses and had to be admitted to a hospital in Bloemfontein.
“I was lucky, and I am still fortunate to be able to afford a psychiatrist and receive the correct medication. However, what happened to me is happening to a lot of people because patients are seen by healthcare providers who refuse to listen and learn.
“I mean, patients are referred to Mohlomi by general practitioners from different health facilities, only to be treated by other general practitioners. That is a recipe for disaster,” she said.
The assertion that Mohlomi Mental Hospital patients are attended to by general practitioners was confirmed by Rampeta, who informed Newsday that the hospital has only one psychiatrist who sees patients once a week. She stated that patients are primarily seen by general practitioner doctors.
Additionally, the Ombudsman disclosed that the hospital lacks professional expertise and suffers from systemic failures that perpetuate human rights abuses.
“The hospital remains the only psychiatric hospital in the country; however, it currently operates without any resident psychiatrists. It has been determined that the sole psychiatrist who previously worked at the hospital left in 2016/2017 for similar reasons.”
The report further indicated that the hospital currently relies on three general medical officers, four psychologists, and seven social workers. It also identified a need for occupational therapists, which the hospital currently lacks.
During the inspection visit, the Ombudsman was informed that the hospital now receives assistance from one psychiatrist from Partners in Health (PIH), a partner of the Health Ministry. This psychiatrist visits the facility once a week, and this arrangement has been in place since December 2022. However, the Ombudsman discovered that the psychiatrist’s scope of work is limited to general patients.
Meanwhile, Liteboho recounted her experiences of a three-month admission, during which she would relapse as though she was not on her medication.
“I never relapse because I stopped my treatment, but when my mental health strikes, it cares not where I am or if I have taken my medication. It seems as if the medication doesn’t work and there is no one willing to explain why I keep falling off the same wagon despite being on treatment,” she says.
Mental Health Association raises concerns
‘Mathabang Manamolela, a former nurse and current president of the country’s Mental Health Association, expressed her concerns in an interview with Newsday.
Manamolela stated that, as a former employee of the hospital, she knows that the seclusion room is used to ensure the safety of patients and staff.
However, she found the reported incidents alarming and pledged to take action: “What you have told me is terrible. We have a close relationship with the ministry, and I promise you that we are going to take this up and demand that an investigation be lodged because the hospital is supposed to be helping mental health patients get better and not worse.”
She quickly pointed out that since leaving, the situation at the hospital has worsened: “We continue to hear that the hospital is severely understaffed and lacks the specialists needed to adequately assist patients.”
She added: “What one can infer is that, given the poor working conditions, the workers may also be experiencing depression. There is much work to be done, and with the help of the stories you share as the media, our advocacy efforts will be strengthened.”
Manamolela emphasised that while they advocate for policy changes and improved services, they strongly disapprove of any abusive acts towards patients. She also highlighted the old and dilapidated condition of the hospital building, urging the Ministry of Health to take intentional action to help improve the hospital.
Meanwhile, Rampeta also stressed on the importance of improving the infrastructure, citing that the state of the seclusion rooms is devastating and perpetuating inhuman treatment on their own.
“The rooms are very old and in devastating condition. The beds don’t have mattresses, forcing us to always have a mattress ready for when a patient is sent to the seclusion rooms.”
This article was investigated and produced by Newsday Media on 16 February 2024 – https://newsdayonline.co.ls/mohlomi-hospitals-reign-of-terror/.
Disclaimer: All patient names mentioned in this article have been changed to protect their privacy and confidentiality. By using pseudonyms for the patients, such as Reitumetse Mohai and Liteboho Sekhamane, their identities remain anonymous while still allowing their experiences to be shared for the purpose of raising awareness about alleged human rights violations at the hospital.

