Empowering Africa: Newborn Screening and Policy Recommendations to Tackle Rare Genetic Conditions
12 February 2024 by Pascalinah Kabi
Est Read Time: 9 min(s) 34 sec(s)

Credit: The Plight of Rare Diseases in Southern Africa: Health and Social Services Policy Recommendations.
“I would be told to do squats as punishment. But I cannot even do simple squats, my medical condition doesn’t allow me.”
Amidst the hustle and bustle of the school day, 15-year-old Khauhelo Olcima Molahli finds himself in a precarious position.
Less than 13 years ago, Molahli’s life took a dramatic turn. Rushed into the emergency room at Queen Elizabeth II Hospital in Maseru, he was barely two-years-old.
With doctors working tirelessly to assist him, Molahli was soon transferred to Bloemfontein, South Africa, for thorough medical tests.
It was there that Molahli’s mother received the devastating news: her son has a rare disease – haemophilia.
Haemophilia is a rare condition that one is born with. This genetic disorder can occur when the body lacks certain proteins called clotting factors.
Haemophilia: A serious challenge in Lesotho
Dr. Lucy Mapota, a director of clinical services at the Ministry of Health, underscores the gravity of haemophilia in Lesotho.
“Haemophilia is a serious challenge in Lesotho,”” explains Dr Mapota, adding “It is a rare blood disease and remains a significant problem in our country.”
Because of the souring cases of haemophilia in Lesotho, Dr. Mapota says the country should move towards screening male newborns to enable parents to know what they are dealing with.
“We still don’t have the capacity to do newborn screening for genetic issues,” Dr. Mapota. She quickly adds that newborn screening for haemophilia, a genetic disorder, would enable Lesotho parents to know that they must rush a child to the hospital as soon as possible if they fall and bleed while playing.
Dr. Mohamed Zahir, a Tanzanian molecular geneticist specialising in the study of genes and their functions at the molecular level, sheds light on newborn screening.
“Newborn screening is a process whereby the moment a child is born, doctors take small samples of a child’s blood and test it for genetic mutations that they think a child might be carrying,” Dr. Zahir explained.
“In that sense, newborn screening allows us to basically determine in advance if a child is carrying any genetic mutation or any discrepancies in the DNA sequence of the child,” Dr. Zahir said, adding “so that in the future, based on what we find in that DNA information, we can tell whether or not the child will be susceptible to a certain disease.”
He explains that newborn screening is beneficial early on because upon diagnosing the newborn child, you immediately discern whether the child carries a mutation for the disease or is a carrier.
Dr. Zahir elaborated in an exclusive interview with Uncensored News on 26 January 2024 that having this information enables individuals to adjust their lifestyles proactively. He adds that newborn screening also allows doctors to administer medication pre-emptively before any symptoms of genetic disorders manifest in the child.
In simple terms, Dr. Zahir explains, “so you delay the onset of the disease, or you know if she/he is the carrier of a certain disease.”
Also read: https://www.uncensored.org.za/empowering-communities-tanzanias-dr-mohamed-sahir-explores-the-role-of-newborn-screening-in-africas-healthcare-landscape/
For individuals who are carriers of genetic disorders, there is a risk of passing the disease on to their children later in life. Therefore, if carriers are screened at birth, they can inform their partners about this later on in life.
If both parents are carriers, Dr Zahir explains that there is a high likelihood that their child will inherit a genetic disorder.
“Newborn screening allows doctors to provide genetic counselling to the parents or the entire family very early on in their lives, before even a patient has exhibited the symptoms.
“Early or newborn screening provides avenue for early detection of genetic conditions but also mitigation efforts including lifestyle changes, early medication and so on,” Dr. Zahir explained.
“I was 1 year, 6 months old when doctors informed my parents that I have haemophilia.”
However, despite its evident benefits, Dr. Zahir observes that newborn screening is not as routinely practiced in Africa because of multiple factors like financial constraints.
In a separate interview, Dr. Lucy Mapota acknowledges the financial barriers hindering Lesotho’s aspirations for newborn screening.
“As a country, we first have to decide which genetic diseases to screen in newborn babies because it is very expensive to carry out genetic newborn screening,” she noted.
“Screening for a genetic disease that affects only one person in a year may be too expensive for the country and could actually make other people suffer because a significant portion of resources would be invested in a program that can detect one genetic disease in one person per year.”
However, she swiftly acknowledges the necessity of screening for prevalent genetic diseases like haemophilia in Lesotho, nothing the need for the country to move towards birth screening for haemophilia.

Founder of Rare Diseases Association Lesotho, Nthabeleng Ramoeli. Credit: Nthabeleng Ramoeli.
Nthabeleng Ramoeli, a staunch advocate for rare disease patients in Lesotho, regards newborn screening as a pivotal mechanism in addressing rare conditions in the country.
“On an international stage, one thing that has significantly benefited many communities dealing with rare diseases is newborn screening,” emphasises Ramoeli.
She adds: “The notable advantage of newborn screening is that it doesn’t only identify rare conditions but also proves invaluable in managing them effectively.”
15-year-old Khauhelo Olcima Molahli reveals that his family only learned about his rare genetic disorder when he was 18 months old.
“I am told that I was one year and six months old when my parents took me to Queen II Hospital. I was transferred to Bloemfontein because local doctors could not diagnose my condition,” recounts Molahli.
Today, Molahli, a Grade 10 student at Leqele High School in Maseru, finds solace in his studies despite facing significant challenges with punishments at school.
“Sometimes I would be told to do squats as punishment, but I cannot because I know my joints will be very painful. It pains me a lot when I sometimes get accused of not wanting to do anything. I did not choose to have this condition,” Molahli expressed.
The hallmark clinical characteristics of haemophilia include bleeding into major joints such as ankles, knees, and elbows, which can occur spontaneously or due to trauma. Molahli expresses discomfort at living with a condition that confines him indoors.
“I am multitalented, I love football, but I cannot play it because of my condition. I just sit indoors,” he lamented.
Ramoeli advocates for newborn screening
Ramoeli is the founder of Rare Diseases Association Lesotho. Ramoeli, who herself lives with a rare connective tissue disorder, believes that newborn screening can equip parents of newborns with rare conditions to navigate their child’s health journey with greater preparedness, thereby alleviating some of the burdens they face.
“I genuinely believe that if I had been diagnosed earlier, my quality of life would likely have been better. Younger children with my rare condition are leading fulfilling lives because they were aware of what their bodies should and should not do from an early age,” reflects Ramoeli.
She added: “They already understand what they can and cannot do. I cannot imagine the stuff my body did that should not have happened if I knew I have this condition.”
Moreover, Ramoeli underscores, “I am a huge advocate for newborn screening. If I were asked what one thing I would prioritise if money was not a problem, it would be to ensure the implementation of newborn screening in Lesotho’s healthcare facilities, and across the entire African continent.”
While Ramoeli acknowledges that newborn screening cannot cure rare conditions, she staunchly believes it should be a mandatory practice in Africa.
“It would significantly benefit individuals living with rare conditions and their parents, providing early detection and thereby easing the emotional turmoil associated with denial,” she explained.
Ramoeli reflected on her own journey, noting, “Newborn screening could have expedited my parents’ acceptance of my condition. Denial is a natural response, and my mother grappled with it initially, reluctant to acknowledge my diagnosis despite seeking medical advice.”
Tanzania leads the way in newborn screening and rare disease advocacy
The study, ‘Empowering newborn screening programs in African countries through establishment of an international collaborative effort,‘ highlights the importance of newborn screening. Despite being commonplace in developed nations since the early 1960s, newborn screening still only reaches about one-third of the world’s newborns.
The study notes that newborns in countries with low- and middle-income economies often undergo screening for only a single condition, while those in higher-income countries may be screened for over 50 conditions.

Dr Mohamed Zahir, third from left, attended a national human genetics stakeholder meeting co-organised by Tanzania Human Genetics Organisation and National Institute for Medical Research. Credit: Aneth David.
Dr. Mohamed Zahir, a molecular geneticist, elaborates on Tanzania’s strides in genetic screening for sickle cell disease in newborns, attributing it to robust research efforts, training, and awareness campaigns.
These efforts align with broader policy recommendations aimed at improving healthcare services for individuals with rare diseases.
“We have initiated a newborn screening program, focusing particularly on sickle cell disease,” he explains. “Sickle cell disease is a monogenic condition caused by a single mutation.”
Dr. Zahir further reveals a concerning statistic about sickle cell disease in Tanzania, stating, “Unfortunately, 50 percent of these children succumb to the disease before reaching the age of five.”
The aim of the newborn screening initiative, according to Dr. Zahir, is to promptly identify affected children or carriers immediately after birth.
This enables early initiation of appropriate treatments such as immunizations, hydroxyurea, and lifestyle adjustments, ultimately improving patient outcomes.
In December 2023, the Food and Drug Administration in the United States approved a treatment for sickle cell disease, a debilitating illness affecting over 100,000 Americans, with a majority being Black. This therapy marks the first medicine approved in the United States that utilises the gene-editing tool CRISPR, recognised by the Nobel Prize in Chemistry in 2020 for its inventors.
Though this treatment has yet to reach Africa, Dr. Zahir emphasises that identifying carriers of sickle cell disease through newborn screening contributes to informed family planning decisions, thereby bolstering disease prevention strategies.
Meanwhile, Tanzania’s commitment to rare diseases extends to the introduction of a specific health budget. Dr. Zahir explains that this progressive policy was adopted following collaborative efforts between organisations such as the Tanzania Human Genetics Organisation and the Ali Kimara Foundation.
“A few years later, the Tanzanian government came forward and established a specific budget within the Ministry of Health, which is now supposedly going to be used to buy the drugs required for these patients,” Dr. Zahir said.
“The funding will also be used to provide diagnosis to these patients and in certain instances, the government will also pay for homeschooling because some patients are okay to study but have special requirements.”
In Lesotho, 15-year-old Khauhelo Olcima Molahli aspire to be a medical doctor to help and advocate for children with rare diseases. Molahli shares his personal experience living with haemophilia and his determination to make a difference.
“Living with haemophilia is seriously challenging,” Molahli shares.
“Besides not being able to play physical games with boys my age, I have to self-administer my injections. Previously, I did not know how to inject myself, but now I know. These are some of the things that I strongly feel that other patients should have access to.
“This is why my goal is to become a medical doctor so that I can help other patients in my condition. I also want to advocate for their rights because currently, most people do not understand that we did not choose to have a condition that is incurable.”
Dr. Zahir emphasises the importance of partnerships with government institutions and professional bodies to amplify the voices of affected individuals and address the challenges surrounding rare diseases.
“(Patients and caregivers can navigate challenges around rare diseases) by engaging in mass awareness or high-level advocacy,” he argues, stressing the need to break the silence and raise awareness about the issues faced by patients and their families.
Calls for centralised care in southern Africa
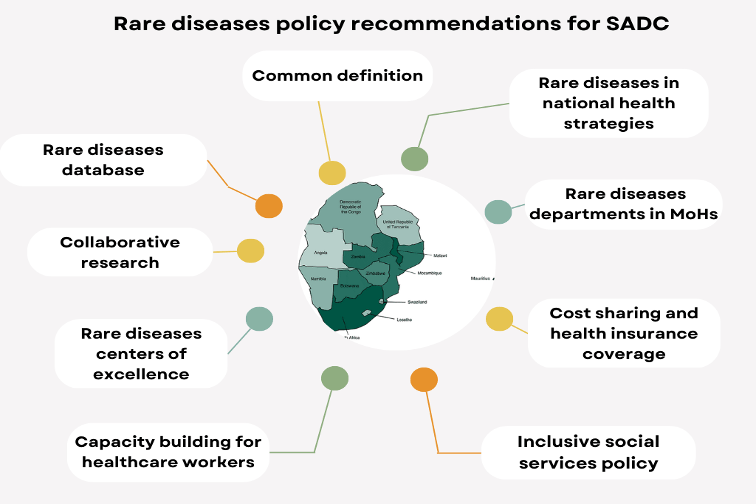
Credit: The Plight of Rare Diseases in Southern Africa: Health and Social Services Policy Recommendations
In 2023, a coalition of professional human genetics organisations, rare disease patient advocacy groups and the health youth cluster from six African countries published a position paper on the status of rare conditions in sub-Saharan Africa.
Ramoeli and Dr. Zahir are two of the six co-authors of the article – ‘The Plight of Rare Diseases in Southern Africa: Health and Social Services Policy Recommendations’ – which highlights that policy frameworks on rare diseases in sub-Saharan Africa are either non-existent or fragmented.
This position paper argues that rare diseases are understudied and are difficult to diagnose, manage, and treat.
“The situation is worse in sub-Saharan Africa (SSA), where the public health infrastructure is weak, leaving a high health and cost burden on patients and caretakers,” the paper states.
“SSA is yet to adopt a common definition of what constitutes a rare disease as other regions, let alone establish the demographics of the kinds of rare diseases afflicting the population and the actual burden.”
More worryingly, the paper has established that policy frameworks and instruments to guide the management of rare diseases are non-existent. It notes that this gap contributes to a slow pace in the realization of universal healthcare and the sustainable development goals in this region.
“We propose the adoption of a unified approach to tackle the burden of rare diseases across the SADC (Southern African Development Community) region by implementing common policies and measures aimed at improving the health and livelihood of people living with rare diseases,” the paper recommends.
“The recommendations include adopting a common definition, centralizing healthcare services, adopting preventive approaches, fostering collaborative research, and capacity building for healthcare workers,” it further suggests.
“In addition, we propose shared cost-bearing models and special health insurance coverage that will ensure the provision of needed health and social services that improve the lives of people living with rare diseases,” reads the paper.



4 Comments
Wow Thanks for this site i find it hard to come across good quality important info out there when it comes to this content appreciate for the post website
I don’t think the title of your article matches the content lol. Just kidding, mainly because I had some doubts after reading the article.
Many thanks for posting this interesting article. I found some really useful points here. Great job, and I hope to see more from you soon.
This is a very clear post. As someone who manages content, I found this especially applicable. If you’re interested, I recently wrote something related on my site too. Keep up the solid work!